Doctor Rids NLR Man of Barrett’s Disease
| July 18, 2017 | A year ago, Reg Hamman of North Little Rock was convinced he had heart problems. There was discomfort in his chest that prompted him to visit his cardiologist.
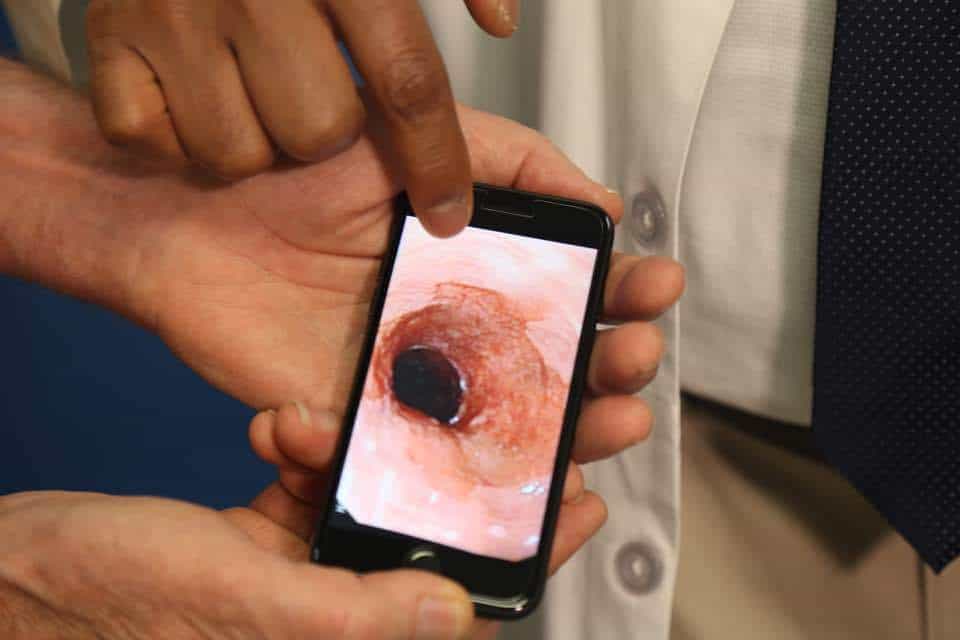
“It turns out it was acid reflux,” Hamman said. “I was referred to my gastroenterologist who found out through an endoscopy that I had Barrett’s esophagus. I’d never even heard of Barrett’s before. Now suddenly I had it.”
Barrett’s disease is a relatively common pre-cancerous condition in patients with heartburn caused by the repeated exposure of the esophagus to acid refluxing from the stomach. It occurs in about 7 percent of people over age 40 .
Hamman, 71, is a zealous learner. He spent a lot of time finding out exactly what Barrett’s disease is, how to treat it, and which doctor he should see.
“I did a lot of research. I found several different states that had physicians that did the procedure to get rid of Barrett’s,” Hamman said. “After meeting Dr. Tharian, I felt comfortable UAMS was the place to be. Dr. Tharian explained the procedure carefully and with confidence.” 
Benjamin Tharian, M.D., is an assistant professor and director of advanced endoscopy in the Division of Gastroenterology and Hepatology in the UAMS College of Medicine. He sees patients in the gastroenterology clinic.
“Barrett’s is concerning because it is a pre-cancerous condition,” Tharian said. “It is to the esophagus, what a polyp is to the bowel or a lump to the breast. We want to prevent it from developing into cancer.”
About a decade ago, the only treatments for Barrett’s disease was prescribing acid inhibitors and close monitoring that included endoscopies with biopsies every three years. If any worrying changes are noted in the biopsy under a microscope, patients used to be referred for an esophagectomy (surgery to remove the food tube).
Two revolutionary treatments have come available in the last 10 years: endoscopic mucosal resection (EMR) and radiofrequency ablation (RFA). Tharian is the only physician who offers the combo-treatment in Arkansas. Cryotherapy is done if RFA/EMR fails and esophagectomy would be the last option.

Reg Hamman originally thought he had heart problems because he was experiencing discomfort around his chest. His cardiologist ruled it out and referred him to a gastroenterologist who diagnosed him with Barrett’s esophagus, a pre-cancerous condition. Hamman later scheduled treatment with Benjamin Tharian, M.D. to remove the Barrett’s disease.
In EMR, the physician removes abnormal tissue from the esophagus through an endoscope after applying a band. For the radiofrequency ablation, Tharian uses an electrode mounted on a balloon catheter or a metal plate. The ablation coagulates the lining, which Tharian then removes. The scar from the ablation heals with normal tissue in a few days to few weeks. This is an outpatient procedure and the patient is able to eat regular food as early as three to five days depending on their symptoms. Side effects and complications are minimal.
“During his last endoscopy about a month ago (about a year after finding the Barrett’s Disease), we took multiple biopsies at different levels to look for any hidden glands or any changes. There is none at all. That’s the way we confirmed his Barrett’s was gone.”
Tharian says the procedure is successful in removing Barrett’s more than 80 percent of the time and eliminates the high-risk dysplastic tissue almost always. Patients will continue to be monitored long term for recurrence of the disease.
and eliminates the high-risk dysplastic tissue almost always. Patients will continue to be monitored long term for recurrence of the disease.
“The whole experience has been educational and positive,” Hamman said. “I feel great and I’m thankful that I’m healed.”